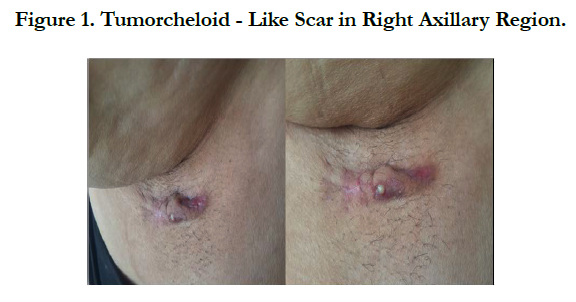
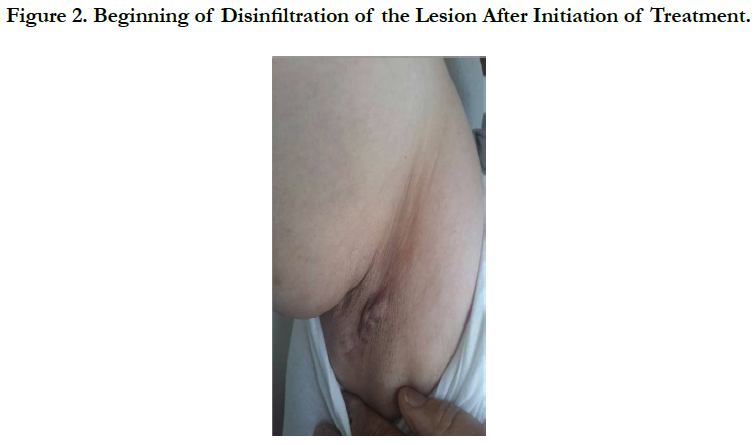
First Case of Chromoblastomycosis From Morocco
Elloudi S1*, Lahlou A1, Gallouj S1, Tlamçani Z2, Mernissi FZ1
1 Department of Dermatology and Venereology , University Hospital Hassan II Fez, Morocco.
2 Centre of mycology, University Hospital Hassan II Fez, Morocco.
*Corresponding Author
Sara Elloudi
Department of Dermatology and Venereology,
University Hospital Hassan II Fez, Morocco.
Email: saraelloudi@gmail.com
Article Type: Case Report
Recieved: November 21, 2016; Accepted: December 29, 2016; Published: December 30, 2016
Citation: Elloudi S, Lahlou A, Gallouj S, Tlamçani Z, Mernissi FZ (2016) First Case of Chromoblastomycosis From Morocco. Int J Microbiol Adv Immunol. 04(2), 75-76. doi: http://dx.doi.org/10.19070/2329-9967-1600014
Copyright: Elloudi S© 2016. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution and reproduction in any medium, provided the original author and source are credited.
Abstract
Chromoblastomycosis is a rare, chronic, fungal infection of the skin and subcutaneous tissues caused by dematiaceous (black) fungi living as saprophytes on plants or vegetable debris in the soil. The lesions are located mainly at the extremities. To the best of our knowledge, wehere in report a first case of chromoblastomycos is from Morocco with an atypical localization.
2.Introduction
3.Case Report
4.Discussion
5.References
keywords
Chromoblastomycosis; Dematiaceous Fungi; Terbinafine.
Introduction
Chromoblastomycosis is a rare, chronic, fungal infection of the skin and subcutaneous tissues caused by dematiaceous (black) fungi living as saprophytes on plants or vegetable debris in the soil. The causative agents are most often three fungal species: Fonsecaea pedrosoi, Phialophora verrucosa and Cladophialophora carrionii. Chromoblastomycosis has a worldwide distribution but is mostly seen in tropical and subtropical zones with high incidence in endemic areas. To the best of our knowledge, wehere in report the first case of chromoblastomycosis from Morocco.
Case Report
A 56-year-old woman, with history of diabet consulted our department for a right axillary lesion that was presenting a progressive growth for one year, and the patient denied previous trauma. Physical examination revealed a tumor cheloid-like scar in here right axillary region, pinkish in color, measuring 3 centimeters in major axis . In the direct mycological examination with 20% KOH, the research for fungal structures was negative. A biopsy of the lesion was performed and anatomopathological studies showed epidermis with moderate irregular acanthosis and dermis presenting lymphohistiocytic infiltrate, and some giantcells. Culture of fragment of the material in Sabouraud agar showed growth of nonspecific dematiaceous cottony colony and micro cultivation showed Cladosporium Sp, confirming the hypothesis of chromoblastomycosis. The patient was treated by terbinafine 500
mg/day for 6 months with good improvement.
Discussion
Chromoblastomycosis is a chronic subcutaneous mycosis that predominantly occurs in tropical and subtropical regions [1]. It mainly affects men living in rural areas and aged between 30 and 60 years, who likely acquire the infection by traumatic inoculation while working [2].
The lesions are characterized by slowly expanding nodules that eventually lead to emerging, cauliflower-like, mutilating and disfiguring eruptions and their severity is divided into mild, moderate and severe forms [3]. Differential diagnosis depends on clinical presentation. It typically includes scars, psoriasis, tumoral nodules and inoculation disease [4].
In our patient, considering evolution gummy and axillary location, other diagnosis were suspected specially scrofuloderma tuberculosis. The causative agents are dematiaceous fungi living as saprophytes of decaying wood and plants. Cladosporium carrionii is the most frequent agent in tropical zones found in Venezuela, in Australia, SouthAfrica, and Mexico chromoblastomycosis confirmed by histologic study and whose agent was identified by myclogical culture and micromorphology [5]. Many therapeutic approaches have been reported, including intravenous or oral antifungals, surgical excision, and physical treatments, used alone or in combination [6]. However, there is currently no gold standard therapy for chromoblastomycosis. For our patient, oral therapy with terbinafine during 6 months was a good option as here lesion was small.
References
- Verrinder Veasey J, Facchini Lellis R, Clarisse Zaitz, Muramatu LH, Machado Bde A (2015) Tumoral chromoblastomycosis: a rare manifestation with typical complementary exams. An Bras Dermatol. 90(6): 907-8.
- Torres-Guerrero E, Isa R, Isa M, Arenas R (2012) Chromoblastomycosis. Clin Dermatol. 30(4): 403–438.
- Ameen M (2009) Chromoblastomycosis: clinical presentation and management. Clin Exp Dermatol. 34(8): 849-854.
- Queiroz-Telles F, Esterre P, Perez-Blanco M, Vitale RG, Salgado CG, et al., (2009) Chromoblastomycosis: an overview of clinical manifestations, diagnosis and treatment. Med Mycol. 47(1): 3–15.
- Hirak Jyoti Raj, Banashree Majumdar, Atul Jain, Prasanta kumar Maiti, Gobinda Chatterjee (2015) A Clinico-Mycological Study on Suspected Cases of Chromoblastomycosis: Challenges in Diagnosis and Management. J Clinical Diagn Res. 9(12): 01-04.
- Tanuma H, Hiramatsu M, Mukai H, Abe M, Kume H, et al., (2000) Case Report. A case of chromoblastomycosis effectively treated with terbinafine. Characteristics of chromoblastomycosis in the Kitasato region, Japan. Mycoses. 43(1-2): 79–83.